 Almost all cervical cancers are caused by a virus called the human papillomavirus (HPV). HPV is spread sexually and is very common so about 80% of sexually active people are infected in their lifetime. Most people will clear the virus but for some people it can persist and cause changes in the cervix which can eventually lead to cervical cancer.
Almost all cervical cancers are caused by a virus called the human papillomavirus (HPV). HPV is spread sexually and is very common so about 80% of sexually active people are infected in their lifetime. Most people will clear the virus but for some people it can persist and cause changes in the cervix which can eventually lead to cervical cancer.
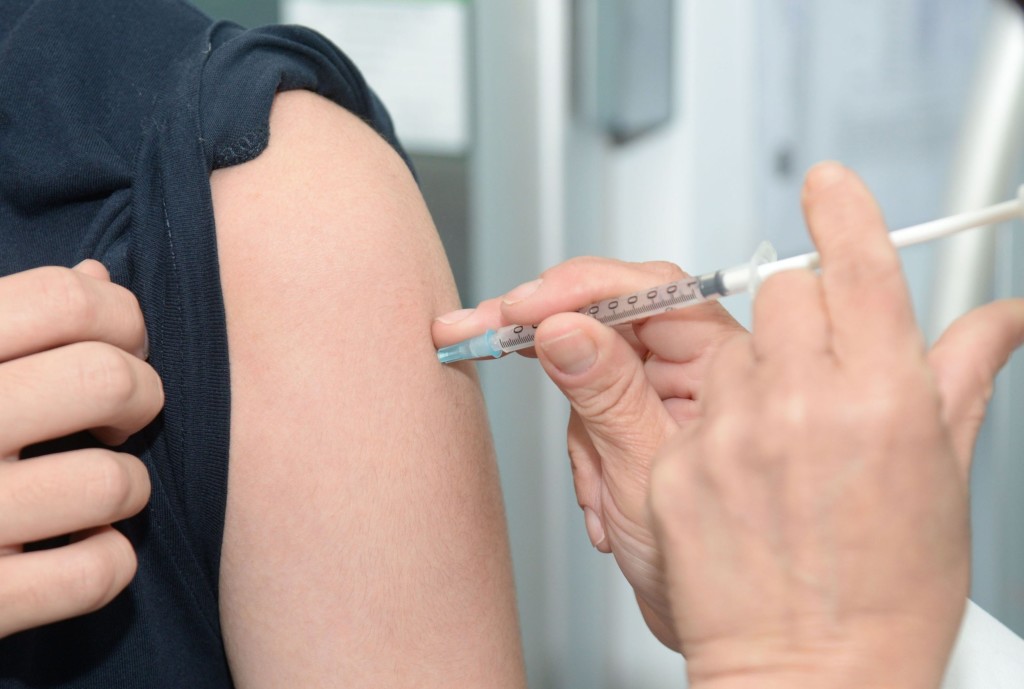
The HPV vaccination programme started in the UK in 2008 and so far, more than 10.5 million doses have been given to girls aged 12/13. The vaccine protects against the most common types of high risk HPV which can cause cancer and also against the low risk types of HPV which can cause genital warts. It is important to vaccinate children before they become sexually active as the vaccine prevents the virus from entering the cells of the cervix but cannot help clear the virus once it is already in the cells.
A study published in The Lancet has hit the headlines recently as it has shown that there has been an 83% reduction in infection rates with high risk HPV. Rates of genital warts have reduced by 67% and rates of moderate precancerous changes in the cervix (CIN2) have decreased by 51%.
A reduction in cervical cancer has not yet been seen as there is a long time period between being infected with HPV and developing cervical cancer. However, the vaccine is predicted to dramatically reduce numbers of patients being diagnosed with cervical cancer in the future. It is still important for women to attend cervical screening as the vaccine does not cover all of the types of HPV.
REFERENCES
-
Drolet M, Benard E, Perez N, et al: Population-level impact and herd effects following the introduction of human papillomavirus vaccination programmes: updated systematic review and meta-analysis. Lancet, 2019
